7 July 2025
No Comments
iHuman assignment
NRNP 6541 case week #7 abdominal pain
15 y/o
5′ 8″ (173 cm)
148.0 lb (67.3 kg)
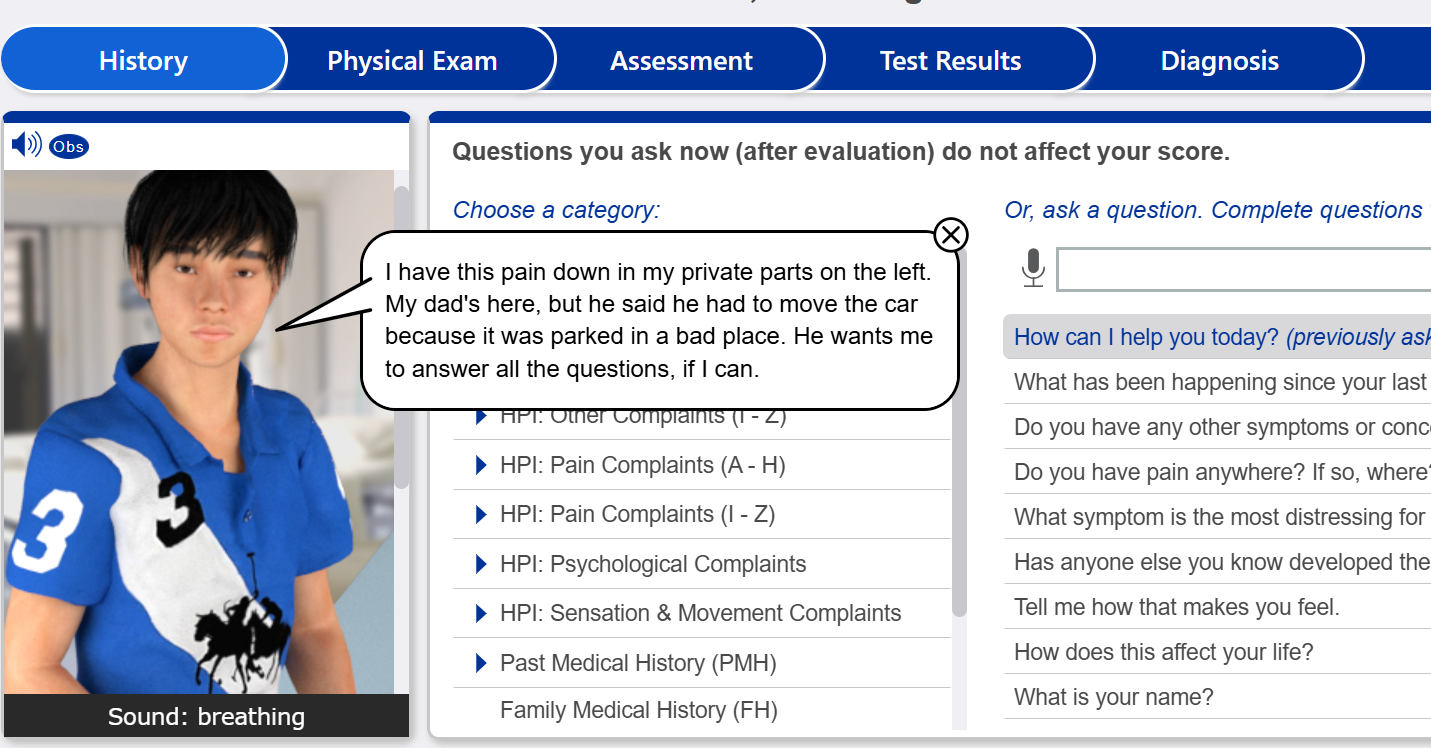
Reason for encounter
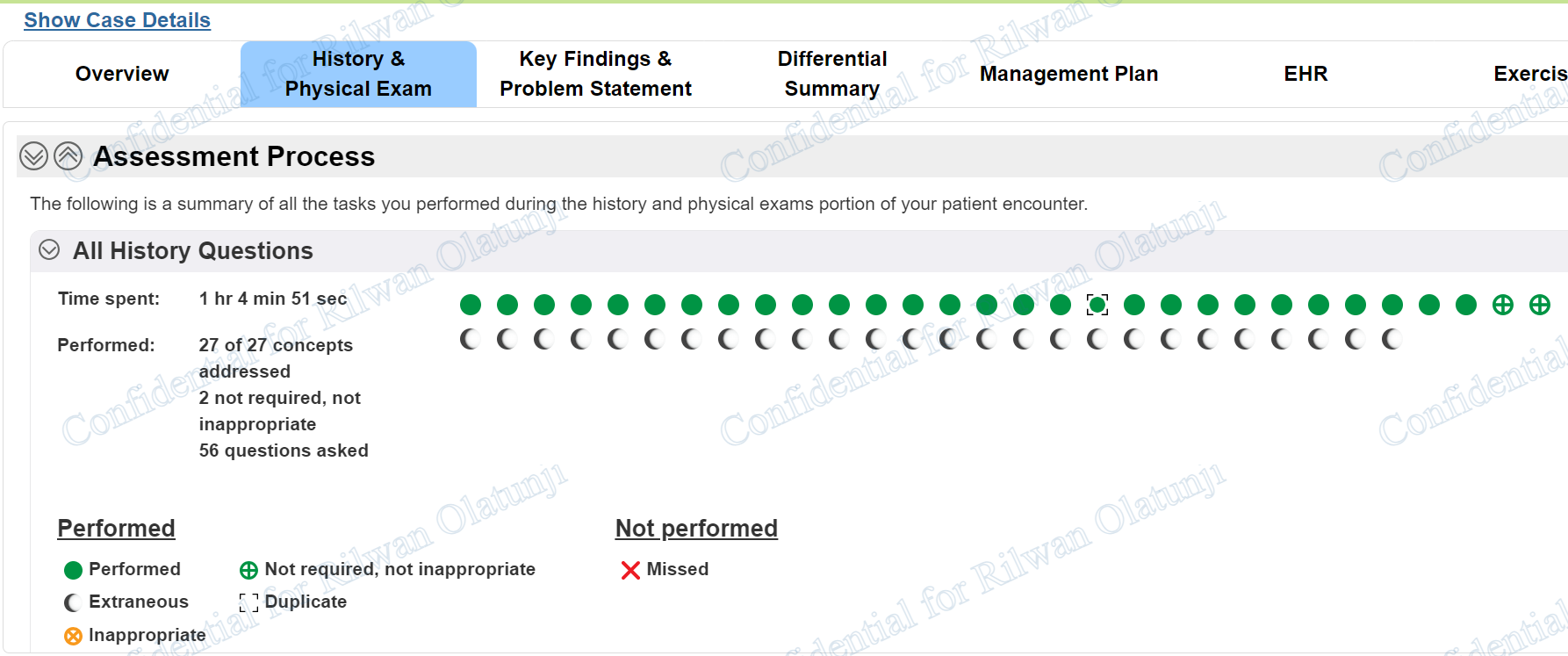
Abdominal painInterview History Questions
- What is your name?
- How can I help you today?
- Do you have any other symptoms or concerns we should discuss?
- Do you have pain anywhere? If so, where?
- What symptom is the most distressing for you?
- Tell me how that makes you feel.
- How does this affect your life?
- Have you gained or lost weight unintentionally, despite normal appetite and exercise?
- ………….
Physical Exams Required
- Weight
- Height
- cognitive status
- SpO2
- temperature
- blood pressure
- pulse
- respiration
- temperature
- auscultate heart
- auscultate lungs…….